Why might breast reduction surgery be considered?
Breast reduction is a clinical procedure performed to reduce the volume and weight of the breast tissue while repositioning the nipple-areolar complex. This surgery is primarily indicated for the management of physical symptoms associated with macromastia (enlarged breasts), such as persistent musculoskeletal pain in the neck, back, and shoulders, or chronic skin irritation (intertrigo) in the inframammary fold.
Your suitability for a reduction mammaplasty is determined through a comprehensive clinical assessment by Specialist Plastic Surgeon Dr Sophie Ricketts. This evaluation includes a review of your medical history, overall health, and a physical examination to ensure the procedure is clinically appropriate for your anatomy. During your consultation, we will discuss the surgical techniques, recovery expectations, and potential clinical risks, such as changes in nipple sensation or impacts on breastfeeding.
What is the recovery time?
Hospital stays for breast reduction surgery are typically one night. The initial recovery period generally spans two to three weeks, during which most patients can return to sedentary or desk-based work, subject to individual progress and medical clearance. While gentle walking is encouraged early in the healing process to support circulation, strenuous or high-impact exercise is restricted for approximately six weeks to allow adequate healing.
It is important to note that recovery timelines are highly individualised and influenced by factors such as your overall health and the extent of the procedure. While the initial swelling and bruising typically subside within the first month, the final surgical outcome is a gradual process, with tissues and scars continuing to settle for up to 12 months post-operatively.
Can I breast feed after breast reduction?
Generally yes, you will still have milk producing glands that function and open into the nipple. The amount of breast tissue that you have after the surgery is less though, and you should expect to potentially need to supplement your breast milk if breast feeding.
Will my nipples still have feeling after surgery?
Changes in nipple and areolar sensation are a recognised clinical risk associated with breast reduction surgery. Post-operatively, patients may experience a temporary or permanent decrease in sensation, while others may report increased sensitivity or no perceptible change. While the total loss of sensation is clinically rare, the outcome is highly variable.
During your consultation, Specialist Plastic Surgeon Dr Sophie Ricketts will discuss how the surgical repositioning of the nipple-areolar complex may impact these nerve pathways. It is important to understand that sensory changes can continue to evolve throughout the first 12 to 18 months of the healing process as the local nerves recover.
Breast Reduction Surgery: Risks and Complications
Breast reduction (reduction mammoplasty) is a major surgical procedure intended to reduce the volume of breast tissue and skin, and to reposition the nipple-areola complex. All invasive surgery carries inherent risks and potential complications.
General Surgical Risks
-
Anaesthesia Complications: Risks associated with general anaesthesia, including allergic reactions or respiratory and cardiovascular issues.
-
Haematoma and Seroma: The accumulation of blood (haematoma) or clear fluid (seroma) in the breast pocket, which may require surgical drainage.
-
Infection: Post-operative infection at the incision sites or within the breast tissue, which may necessitate antibiotic treatment or further surgery.
-
Deep Vein Thrombosis (DVT): The risk of blood clots forming in the legs, which can be life-threatening if they migrate to the lungs (pulmonary embolism).
-
Poor Wound Healing: Risk of wound breakdown or “spitting” stitches, particularly at the “T-junction” of the incisions. This risk is significantly higher for patients who smoke.
Specific Risks of Breast Reduction
-
Permanent Scarring: Scars are an inevitable result of this surgery, typically occurring around the areola, vertically down the breast, and in the crease underneath. While these fade gradually over about 12 months, the final appearance is unpredictable.
-
Nipple and Skin Sensation Changes: Temporary or permanent numbness or altered sensitivity in the nipples or breast skin is common.
-
Asymmetry: Variations in healing or underlying chest wall structure may result in differences in breast size, shape, or nipple position between the two sides.
-
Fat Necrosis: The death of fatty tissue deep in the skin, which can cause firm, palpable lumps and may require further clinical investigation.
-
Nipple/Areola Loss: In rare cases, the blood supply to the nipple may be compromised, leading to partial or total loss of the nipple/areola tissue (necrosis).
-
Interference with Breastfeeding: Breast reduction surgery involves the disruption of milk ducts and nerves, which may affect the ability to breastfeed in the future.
-
Interference with Mammography: Scar tissue can sometimes make it more difficult to interpret future breast cancer screenings; specialised views with other imaging techniques such as ultrasound or MRI may be required.
Your Consultation Process
A consultation with Dr Sophie Ricketts, Specialist Plastic Surgeon, is a comprehensive clinical assessment to determine your suitability for surgery. This process is designed to ensure you are fully informed of the potential risks, expected clinical outcomes, and available non-surgical alternatives relevant to your circumstances.
In accordance with the Medical Board of Australia’s mandatory guidelines for cosmetic surgery:
-
Clinical Evaluation: Dr Ricketts will assess your medical history and physical anatomy to determine if the procedure is clinically appropriate.
-
Psychological Screening: A mandatory assessment for Body Dysmorphic Disorder (BDD) and psychological readiness is required for all patients.
-
GP Referral: You must provide a valid referral from your General Practitioner prior to your initial consultation.
-
Two-Stage Process: A minimum of two pre-operative consultations is required.
-
Cooling-Off Period: After your second consultation, a mandatory 7-day cooling-off period must elapse before any surgery can be booked or payments made.
Frequently Asked Questions
Will my scars be noticeable?
All surgical procedures result in permanent scarring, which in breast reduction typically follows a “lollipop” (circumareolar and vertical) or “anchor” (inverted-T) pattern. In the initial post-operative months, scars often appear erythematous (pink or red) and firm; however, they undergo a natural maturation process over approximately 12 months, during which they typically soften and fade. The final appearance of scars is subject to individual biological factors and genetic predisposition to healing.
To support optimal scar maturation, Dr Sophie Ricketts provides specific clinical aftercare protocols. These may include maintaining surgical tape for the first six weeks to reduce tension and prevent scar widening, followed by the application of hydrating moisturizers and strict sun protection to prevent hyperpigmentation. In some cases, medical-grade silicone gels or sheets may be recommended as clinical interventions. If hypertrophic scarring or persistent redness occurs, additional management options such as laser therapy or topical clinical treatments can be discussed during your follow-up appointments.
How long does the surgery take?
The duration of a breast reduction procedure, or reduction mammaplasty, typically ranges between 2 to 4 hours, depending on the anatomical complexity and the specific surgical technique required. Factors such as the volume of tissue to be resected, the degree of nipple-areolar transposition, and individual structural considerations will influence the precise operative time.
Following the administration of anaesthesia and completion of the surgery, you will be monitored in a clinical recovery area before being transferred to the ward for a 1 night stay.
What is breast reduction surgery?
Breast reduction, or reduction mammaplasty, is a surgical procedure designed to reduce the volume and weight of the breasts by removing excess glandular tissue, fat, and skin. The procedure also involves repositioning the nipple-areolar complex to a higher, more corrected position on the breast mound. This surgery is frequently indicated for patients experiencing physical symptoms such as chronic neck, back, or shoulder discomfort, or skin irritation within the inframammary fold.
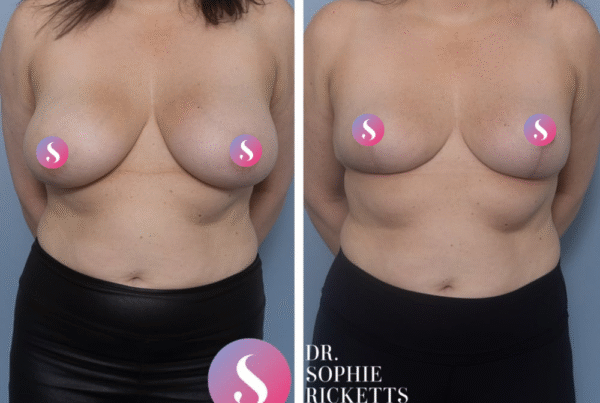
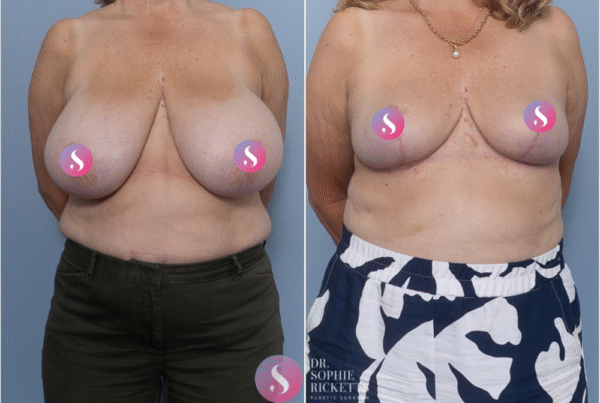
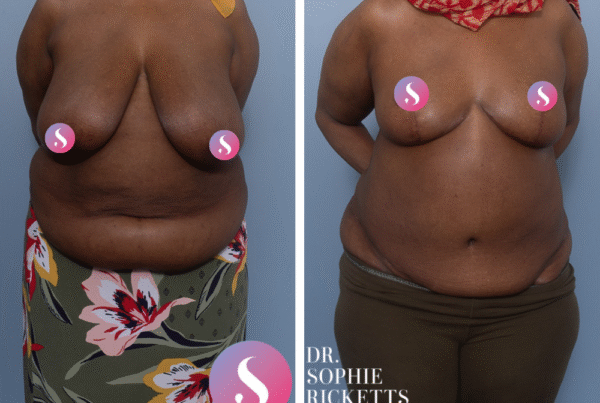
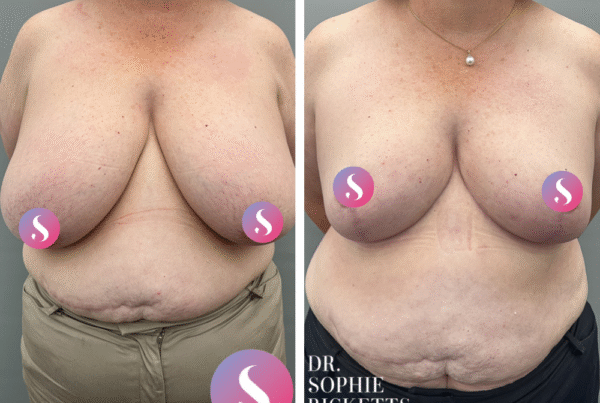
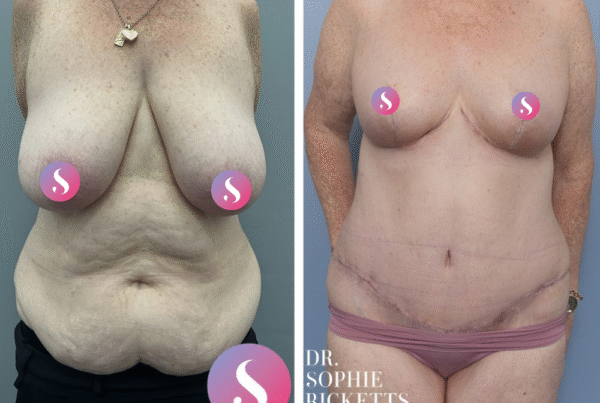
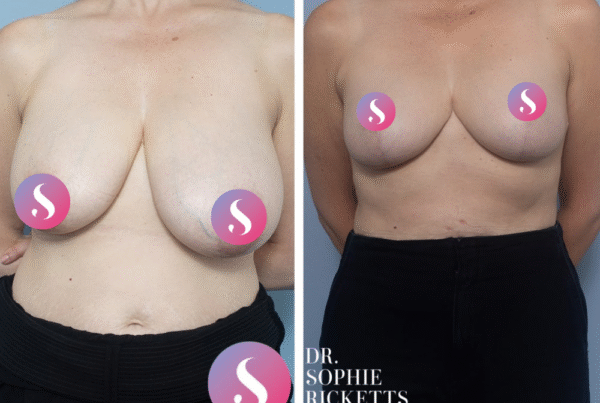
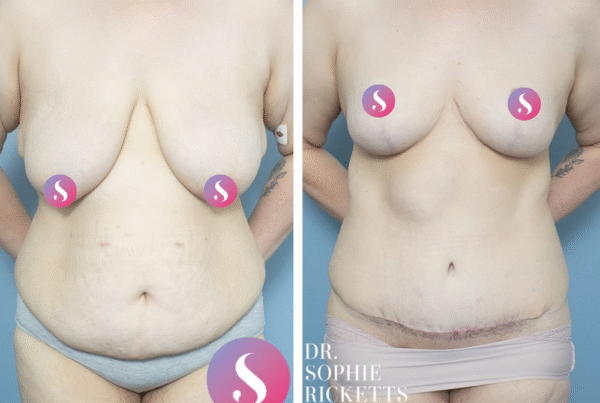
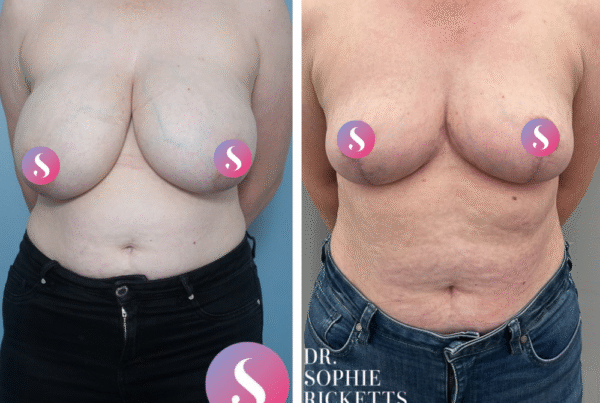
Specialist Plastic Surgeon Dr Sophie Ricketts performs this procedure in Melbourne, Victoria, with a focus on addressing the specific anatomical requirements of each patient. For those considering this surgery, clinical galleries featuring pre-operative and post-operative photographs are available to illustrate potential surgical outcomes and the placement of resulting scars.
A formal consultation is required to assess your suitability for surgery. During this appointment, Dr Ricketts will evaluate your medical history, discuss the technical aspects of the procedure, and outline the inherent clinical risks and expected recovery timeline.
What kind of postoperative care will I need?
After breast reduction surgery, you will need to follow specific postoperative care instructions to ensure proper healing. This includes keeping the surgical sites clean and dry, managing pain with prescribed medications, and limiting physical activity and heavy lifting for several weeks. Wearing any recommended support garments and attending follow-up appointments with Dr Ricketts is crucial for monitoring your progress. Watch for signs of complications, such as infection, and contact your surgeon if any unusual symptoms arise. Proper care also involves avoiding soaking the incisions in water and using treatments to minimise scarring once healed. Following these guidelines will promote a fast recovery and optimal results.
After breast reduction surgery, you will need to follow specific postoperative care instructions to ensure proper healing. This includes keeping the surgical sites clean, managing pain with prescribed medications, and limiting physical activity and heavy lifting in the first 6 weeks. Wearing any recommended support garments and attending follow-up appointments with Dr Ricketts is crucial for monitoring your progress. Watch for signs of complications, such as infection, and contact your surgeon if any unusual symptoms arise. Proper care also involves avoiding soaking the incisions in water and using treatments to minimise scarring once healed. Following these guidelines will promote a smooth recovery.
How do I prepare for breast reduction surgery?
Preparation involves a thorough consultation with your surgeon, where your health, objectives, and medical history are discussed. Dr Sophie Ricketts, a specialist in breast surgery, advises avoiding smoking, certain medications, and herbal supplements that could increase bleeding risks. Arrange time off work, set up your home for recovery, and organise someone to drive you afterwards. You may also need to complete pre-operative tests such as a mammogram.
Am I a candidate for breast reduction surgery?
Clinical suitability for breast reduction surgery, or reduction mammaplasty, is based on the presence of physical symptoms caused by macromastia (enlarged breasts). You may be a candidate for this procedure if you experience chronic musculoskeletal pain in the neck, back, or shoulders, or persistent skin irritation (intertrigo) within the inframammary fold. Functional limitations, such as difficulty exercising or nerve compression (indicated by bra strap grooving), are also key clinical indicators.
As part of the assessment process, Specialist Plastic Surgeon Dr Sophie Ricketts will evaluate your overall health, including factors like Body Mass Index (BMI) and smoking status, which significantly impact surgical risks and wound healing. A referral from your GP is typically required to determine your eligibility for Medicare or private health insurance rebates. This consultation ensures the procedure is a clinically appropriate pathway for your individual anatomy and health profile.
What can I expect during the breast reduction surgery?
A breast reduction, or reduction mammaplasty, is a major surgical procedure performed under general anaesthesia in an accredited hospital. The surgery typically takes between 2 and 4 hours, depending on the volume of tissue being removed and the complexity of the individual anatomy.
The Surgical Process
Marking and Planning: Prior to the administration of anaesthesia, Specialist Plastic Surgeon Dr Sophie Ricketts will complete precise surgical markings on your chest while you are in a standing position. These markings guide the placement of incisions and the new position of the nipple-areolar complex.
- Incisions: Incisions are typically made using a “lollipop” (vertical) or “anchor” (inverted-T) pattern, depending on the degree of reduction required.
- Tissue Removal and Reshaping: Excess glandular tissue, fat, and skin are surgically excised. The remaining breast tissue is then reshaped and lifted to a more elevated position on the chest wall.
- Nipple Repositioning: The nipple and areola are moved to their new, higher position. In the vast majority of cases, they remain attached to their original blood and nerve supply (the pedicle).
- Closure: The incisions are closed in multiple layers using dissolving sutures to support the new breast shape. Surgical tape and a supportive post-operative garment are then applied.
Immediate Post-Operative Care
Following the procedure, you will be monitored in the hospital’s recovery ward by nursing staff. Most patients remain in hospital for one night for clinical observation and pain management. You will wake up wearing a surgical support bra, which must be worn as directed to minimise swelling and support the breasts whilst healing.
Regular follow-up appointments with Dr Ricketts are a mandatory part of the clinical process to monitor your wound healing and ensure the surgical sites are maturing as expected. While initial healing occurs over the first few weeks, the final internal settling of the breast tissue can take 6 to 12 months.
Can I combine breast reduction with other procedures?
In some clinical circumstances, a reduction mammaplasty may be performed in conjunction with another procedure, for example an abdominoplasty.
Clinical Considerations for Combined Surgery
While combining procedures may reduce the total number of individual recovery periods, it significantly increases the duration of general anaesthesia and the overall surgical complexity. The decision to combine procedures is primarily a clinical one, based on your:
- General Health and BMI: Patients must meet strict health criteria to undergo prolonged surgery safely.
- Anaesthetic Risk Profile: Longer operative times carry an increased risk of complications such as Deep Vein Thrombosis (DVT) or pulmonary embolism.
- Wound Healing: Multi-site surgery places a higher demand on the body’s metabolic resources during the initial healing phase.
Consultation and Planning
During your initial consultation, Specialist Plastic Surgeon Dr Sophie Ricketts will perform a comprehensive assessment of your medical history and anatomical goals. If you are considering multiple procedures, it is essential to disclose this so that the cumulative surgical risk can be evaluated.
Dr Ricketts will advise whether a combined approach is clinically appropriate for you or if a staged approach—performing the surgeries several months apart—is the safer and more appropriate pathway for your long-term recovery and surgical outcome.
Will private health insurance cover my breast reduction?
Breast reduction, or reduction mammaplasty, may be eligible for a Medicare rebate if the procedure is performed to address specific clinical symptoms rather than for purely aesthetic reasons. If a procedure meets the strict criteria for a Medicare Item Number, private health insurance funds typically provide coverage for hospital and theatre fees, as well as a portion of the anaesthetic and surgical costs.
Clinical Eligibility (MBS Item 45523)
To qualify for a rebate under MBS Item 45523, the surgery must be considered clinically necessary. This typically requires documentation of:
- Macromastia-related symptoms: Persistent musculoskeletal pain (neck, back, or shoulder) or chronic skin irritation that has not responded to conservative treatments.
- Tissue Resection: A minimum amount of breast tissue (usually at least 500g per breast) must be planned for removal.
- Referral: A valid referral from a General Practitioner (GP) or specialist is mandatory.
Verifying Your Coverage
The level of reimbursement varies significantly between different private health funds and individual policy tiers. Specialist Plastic Surgeon Dr Sophie Ricketts and her team will provide you with the specific MBS item numbers relevant to your proposed surgical plan.
It is the patient’s responsibility to contact their private health insurer to confirm that these item numbers are included in their specific level of cover and to identify any out-of-pocket “gap” expenses.