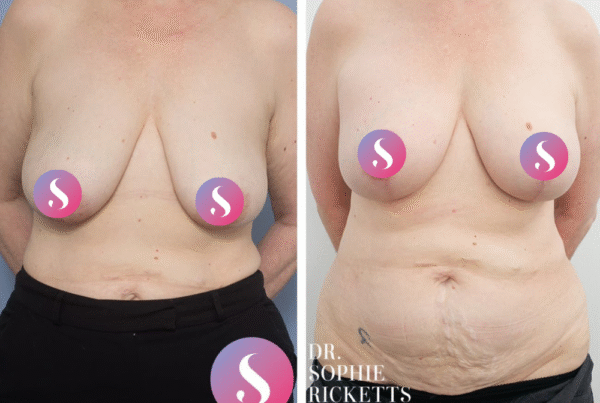
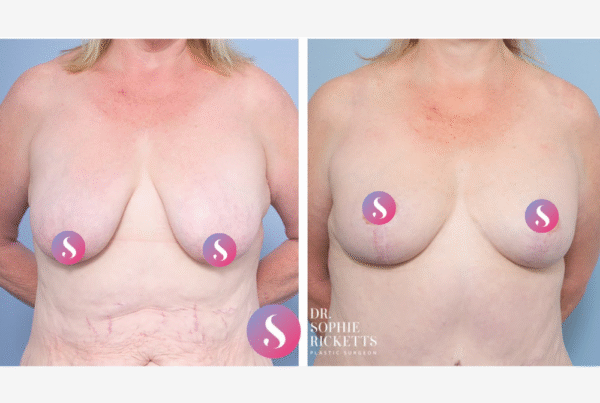
Why might breast lift surgery be considered?
A breast lift, or mastopexy, is a surgical procedure performed to reposition the breast tissue and the nipple-areolar complex to a more elevated position on the chest wall. The primary clinical objective is to correct ptosis by removing excess skin and tightening the surrounding tissue to support the new breast shape.
Clinical Indications for a Mastopexy
Mastopexy is often indicated when there is a significant loss of skin elasticity or a change in breast volume. This typically occurs as a result of:
- Post-Pregnancy and Breastfeeding: Changes in hormone levels and tissue expansion can lead to a loss of structural support once the breasts return to their pre-gestational state.
- Significant Weight Fluctuation: The stretching of the skin envelope during weight gain and subsequent loss can result in redundant skin and tissue descent.
- Age-Related Tissue Laxity: Over time, the Cooper’s ligaments (which support the breast) can stretch, leading to a change in the breast’s position.
Surgical Assessment
Suitability for a mastopexy is determined during a clinical consultation with Specialist Plastic Surgeon Dr Sophie Ricketts. This assessment includes an examination of your breast tissue quality, the degree of ptosis, and your medical history. Dr Ricketts will discuss the different surgical techniques (such as the lollipop or anchor incision patterns), the resulting permanent scarring, and the clinical risks associated with the procedure.
Will I need an implant as well?
A breast lift, or mastopexy, is designed to reposition existing breast tissue and remove redundant skin; it does not add volume to the breast. The clinical decision to include an implant depends on your anatomical goals and the quality of your existing breast tissue.
Mastopexy (Lift Only)
If you are satisfied with your current breast volume but wish to address ptosis (descent) or elevate the position of the nipple-areolar complex, a mastopexy alone may be appropriate. This procedure utilises your own tissue to reshape the breast mound.
Augmentation-Mastopexy (Lift with Implants)
If you wish to increase the volume of the breast or address a loss of fullness in the upper pole (the top section of the breast) that a lift alone cannot achieve, an implant may be discussed.
Will there be scars?
All surgical procedures result in permanent scarring. The extent of the scars depends on the degree of correction required and your individual anatomy. Specialist Plastic Surgeon Dr Sophie Ricketts typically utilises one of three patterns:
- Periareolar: A circular incision around the areola.
- Vertical (Lollipop): A circular incision plus a vertical line to the breast crease.
- Inverted-T (Anchor): Circular and vertical incisions plus a horizontal line along the inframammary fold.
Can breastfeeding be affected after a lift?
Breastfeeding is often possible following a mastopexy (breast lift), but it cannot be clinically guaranteed. The procedure involves repositioning the nipple-areolar complex, which carries a recognised risk of disrupting the underlying milk-delivery structures.
Specialist Plastic Surgeon Dr Sophie Ricketts will discuss these anatomical considerations and individual clinical risks during your consultation.
Will nipple sensation change?
Temporary or permanent changes to nipple and areolar sensation are a recognised clinical risk associated with mastopexy (breast lift). Because the procedure involves repositioning the nipple-areolar complex and altering the surrounding skin, the local nerve pathways are inevitably affected.
Specialist Plastic Surgeon Dr Sophie Ricketts will discuss these neurovascular risks and how they apply to your specific surgical plan during your consultation.
Breast Lift (Mastopexy): Clinical Risks and Complications
A breast lift is a major invasive surgical procedure. While Dr Sophie Ricketts follows rigorous clinical protocols to manage and address potential complications, all surgery carries inherent risks. It is essential for patients to be fully informed of these possibilities before deciding to proceed.
General Surgical Risks
-
Anaesthesia-Related Complications: Potential adverse reactions to general anaesthesia, including respiratory or cardiovascular issues.
-
Haematoma and Seroma: The accumulation of blood (haematoma) or clear fluid (seroma) within the breast tissue, which may require surgical drainage or needle aspiration.
-
Infection: Risk of infection at the incision sites or deeper within the breast tissue, which may require antibiotics or further surgery.
-
Deep Vein Thrombosis (DVT): A higher risk of blood clots in the legs following major surgery, which can be life-threatening if they migrate to the lungs (pulmonary embolism).
-
Poor Wound Healing: Risk of delayed healing or wound breakdown, which is significantly higher for patients who smoke.
Specific Risks of Mastopexy
-
Permanent Scarring: All mastopexy techniques (periareolar, vertical, or anchor) result in permanent scars. The final appearance is influenced by individual genetics and the healing process.
-
Changes in Sensation: Temporary or permanent numbness or altered sensitivity in the nipples, areola, or breast skin is a common clinical outcome.
-
Asymmetry: Variations in healing or underlying chest wall structure may result in differences in breast shape, size, or nipple position between the left and right sides.
-
Nipple or Areola Necrosis: In rare cases, the blood supply to the nipple may be compromised during the repositioning process, leading to partial or total tissue loss (necrosis).
-
Fat Necrosis: The death of fatty tissue deep in the breast, which can result in firm, palpable lumps of scar tissue that may require further clinical assessment.
-
Interference with Breastfeeding: The surgical repositioning of tissue can disrupt milk ducts and nerves, potentially affecting future breastfeeding capability.
-
Recurrent Ptosis: Surgery does not halt the natural ageing process or the effects of gravity; over time, further changes in breast position may occur.
Your Consultation Process
A consultation with Dr Sophie Ricketts, Specialist Plastic Surgeon, is a comprehensive clinical assessment to determine your suitability for surgery. This process is designed to ensure you are fully informed of the potential risks, expected clinical outcomes, and available non-surgical alternatives relevant to your circumstances.
In accordance with the Medical Board of Australia’s mandatory guidelines for cosmetic surgery:
-
Clinical Evaluation: Dr Ricketts will assess your medical history and physical anatomy to determine if the procedure is clinically appropriate.
-
Psychological Screening: A mandatory assessment for Body Dysmorphic Disorder (BDD) and psychological readiness is required for all patients.
-
GP Referral: You must provide a valid referral from your General Practitioner prior to your initial consultation.
-
Two-Stage Process: A minimum of two pre-operative consultations is required.
-
Cooling-Off Period: After your second consultation, a mandatory 7-day cooling-off period must elapse before any surgery can be booked or payments made.
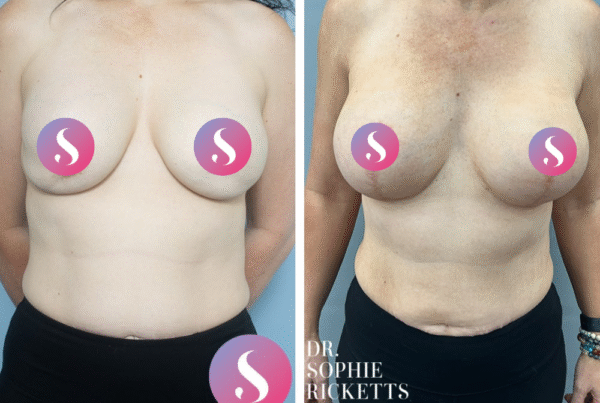
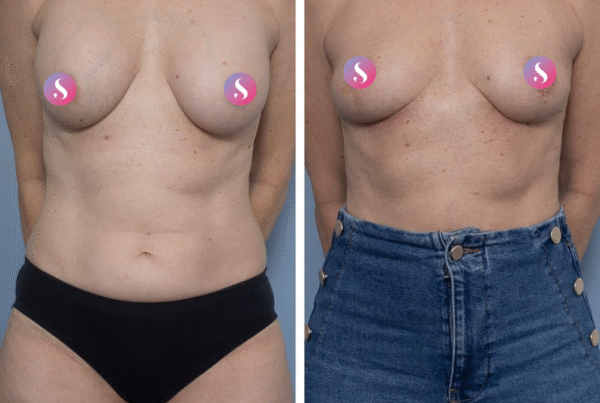
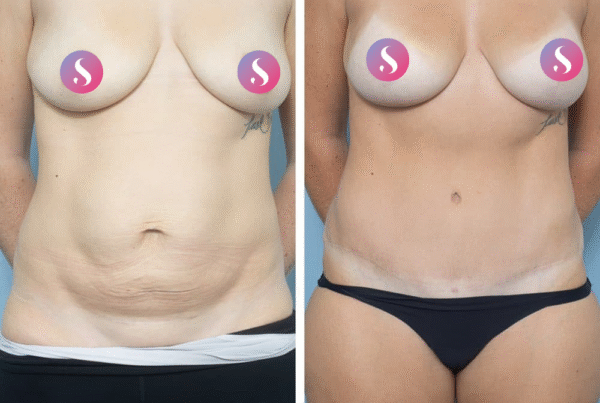
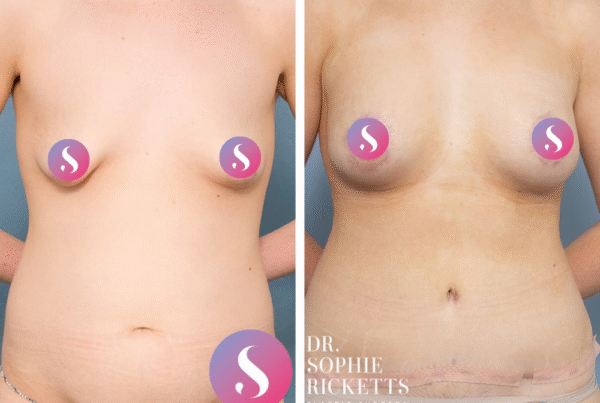
Gallery
Individual results vary. All surgical procedures carry risks and require a consultation to determine suitability.
These images are for illustrative purposes only and do not guarantee a specific outcome. Before proceeding, you should seek a second opinion from an appropriately qualified health practitioner.
FAQ
How do I care for my scars?
Keep incisions clean, dry, and protected from sunlight. Once wounds have closed, silicone gel or sheets may be recommended. Avoid picking at healing skin or using unapproved products. Regular check-ups help ensure your scar-care routine is appropriate for your progress.
What does a breast lift aim to do?
A breast lift (mastopexy) is a surgical procedure that repositions breast tissue and skin. Possible changes from this procedure may include:
- Raising the position of the breasts on the chest
- Changing the shape of the breasts
- Repositioning the nipple and areola
The specific changes vary between individuals and depend on factors such as anatomy, skin condition, and surgical technique.
Important considerations
- Breast lift surgery does not prevent future changes to the breasts over time.
- Outcomes cannot be guaranteed.
- As with all surgery, there are risks, including bleeding, infection, scarring, changes in nipple sensation, and the possibility of further surgery.
A consultation with Dr Sophie Ricketts, Specialist Plastic Surgeon, is required to discuss individual circumstances, potential risks and alternatives, and whether this procedure may be suitable.
What is a breast lift (mastopexy)?
A breast lift, or mastopexy, is a surgical procedure performed to reposition the breast tissue and the nipple-areolar complex to a more elevated position on the chest wall. The primary clinical objective is to address ptosis (descent) of the breast by removing redundant skin and reshaping the breast tissue to achieve a rounder breast contour.
In most cases, the nipple and areola are also repositioned to a higher point on the breast. Specialist Plastic Surgeon Dr Sophie Ricketts utilises tailored surgical techniques—such as the periareolar (around the nipple), vertical, or anchor incision patterns—based on your specific anatomy, the quality of your skin, and the degree of tissue descent.
The procedure is performed under general anaesthesia in an accredited hospital. While a mastopexy addresses the position and shape of the breast, it does not significantly alter the volume; if increased fullness is a clinical goal, an augmentation-mastopexy (lift with implants) may be discussed during your consultation.
At what age can I get a breast lift?
Dr Sophie Ricketts advises that candidates are typically adults whose breast development has fully settled, usually from age 18 onwards. Suitability depends more on general health, stability of breast size, and personal goals than on a specific age limit. During a consultation, she assesses your medical history, lifestyle factors, and desired outcomes.
Are there any risks or complications?
Yes, like any surgical procedure, a breast lift carries certain risks and potential complications. These can include infection, poor wound healing, scarring, asymmetry (uneven results), or changes in nipple sensation, such as numbness or increased sensitivity. In some cases, the breasts may not heal as expected, or the lifted position may not last as long as desired. There is also a possibility of breastfeeding difficulties.
What activities should I avoid after surgery?
Following a reduction mammaplasty or mastopexy, physical activity must be restricted to allow the internal sutures and incisions to stabilise. Specialist Plastic Surgeon Dr Sophie Ricketts provides a structured clinical recovery plan, but generally, the following restrictions apply:
First 2–3 Weeks: Initial Healing
Lifting and Straining: You must avoid lifting any objects heavier than 2–5kg (including children or groceries). Straining can increase blood pressure, which carries a clinical risk of haematoma (internal bleeding).
Overhead Reaching: Avoid reaching high above your head or behind your back, as this places tension on the breast incisions and can lead to wound dehiscence (opening of the wound).
Driving: You should not drive until you are no longer taking prescription pain medication and have regained full range of motion without discomfort—typically at least 10 to 14 days post-surgery.
4–6 Weeks: Tissue Maturation
High-Impact Exercise: Activities such as running, jumping, or heavy gym training must be avoided for at least six weeks. These movements cause breast “bounce,” which can compromise the internal reshaping of the tissue.
Swimming and Bathing: Do not submerge the incisions in baths, swimming pools, or the ocean until they are fully healed and all scabs have naturally separated. This is essential to prevent infection.
Supportive Garments: A medical-grade compression or support bra must be worn 24/7 (as directed) to minimise swelling and support the new breast contour.
Resuming Activity
Dr Ricketts will monitor your progress during mandatory follow-up appointments. She will provide clinical clearance to resume specific activities based on the maturation of your scars and the reduction of post-operative swelling.
Can a breast lift address lower breast position?
A breast lift (mastopexy) is with the aim of repositioning breast tissue and the nipple–areola complex higher on the chest. The specific approach depends on individual anatomy and the degree of tissue and skin change.
How do I know if a breast lift is suitable?
Whether a breast lift (mastopexy) is appropriate can only be determined through a consultation with a Specialist Plastic Surgeon. During this consultation, Dr Sophie will assess factors such as breast shape, skin condition, and nipple position, and will discuss potential risks, alternatives, and whether this procedure may be suitable for you.
How long does recovery take after a breast lift?
Initial recovery usually takes about 2–3 weeks, with many people resuming light daily tasks within a few days. Swelling and tightness improve steadily over about 6 weeks, while full settling can take a few months. Scars generally continue to fade for 12 months or more.
What type of anaesthesia is used during a breast lift?
A mastopexy (breast lift) is a major surgical procedure performed in an accredited hospital. To ensure clinical stability and the necessary surgical conditions, the procedure is conducted under general anaesthesia.
- The Clinical Process
General Anaesthesia: You will be unconscious and under the continuous monitoring of a qualified Specialist Anaesthetist. This ensures that your airway is protected and your vital signs are managed throughout the duration of the surgery. - Local Anaesthetic Infiltration: During the procedure, Specialist Plastic Surgeon Dr Sophie Ricketts may also administer long-acting local anaesthetic into the breast tissue. This is a clinical technique used to assist with post-operative analgesia (pain relief) immediately upon waking.
- Pre-operative Assessment: Prior to your surgery, you will have a consultation or assessment with the anaesthetist. They will review your medical history, including any previous reactions to anaesthesia, current medications, and general health, to formalise a clinical plan tailored to your needs.
Post-Anaesthetic Recovery
Following the procedure, you will be moved to a specialised recovery ward where nursing staff will monitor you as the anaesthetic wears off. Common temporary side effects can include nausea, a sore throat, or drowsiness, all of which are managed clinically in the hospital environment.
Can a breast lift (mastopexy) include changes to the areola?
A breast lift (mastopexy) may include adjusting the size or position of the areola. This is done by removing a measured area of skin around the areola and repositioning it as part of the lift procedure, depending on individual anatomy and the surgical plan.
Whether this is appropriate varies between individuals. During a consultation, Dr Sophie Ricketts will assess your circumstances and discuss the potential options, risks, and alternatives, including whether areola adjustment may be incorporated into your procedure.
What is the difference between a breast lift and breast implants?
A breast lift (mastopexy) is a surgical procedure that repositions breast tissue and the nipple–areola complex to change how the breast sits on the chest. Breast implants, by contrast, are used to change breast volume.
In some situations, both procedures may be performed during the same operation if a change in both breast position and volume is being considered. Whether this is appropriate depends on individual anatomy, overall health, and the extent of the changes desired.
During a consultation, Dr Sophie Ricketts will assess your circumstances, outline the potential risks and alternatives, and discuss which approach may be suitable for you.