What is Breast Augmentation?
Breast augmentation, or augmentation mammaplasty, is a surgical procedure designed to increase breast volume and change breast shape through the placement of breast implants or, in some cases, autologous fat transfer. The procedure involves a clinical assessment of the existing breast tissue, chest wall anatomy, and skin elasticity to determine the most appropriate surgical approach for the individual.
Breast Implant Options
Breast implants are categorised by their filler material, with silicone gel and saline being the two primary options regulated and approved by the Therapeutic Goods Administration (TGA). Silicone gel is the most common filler used in contemporary breast augmentation; following extensive clinical review, regulatory bodies have confirmed its suitability for surgical use. Silicone implants are designed with a cohesive gel that maintains its shape and typically has a lower incidence of palpable rippling compared to saline alternatives.
Saline-filled implants consist of a silicone shell filled with sterile saltwater and remain a clinical option, though they may have a different tactile feel. It is important to note that breast implants are medical devices with a finite lifespan; they are not lifetime devices and may require surgical monitoring, replacement, or removal over time due to clinical factors such as capsular contracture or device depletion. The selection of implant material is determined during your clinical consultation based on your individual anatomy and surgical goals.
What size implant?
The selection of breast implant dimensions—specifically width and height—is primarily governed by your individual chest wall measurements and existing breast tissue envelope. While the volume (measured in cubic centimeters or cc) is discussed in relation to your aesthetic goals, the final selection must be clinically compatible with your anatomical proportions to minimize long-term surgical risks.
Surgical Techniques and Placement
The procedure involves creating a surgical pocket to place the implant. The placement is typically categorised into two primary anatomical positions:
- Subglandular: The implant is placed directly behind the breast tissue and in front of the pectoral muscle.
- Submuscular (Subpectoral): The implant is positioned beneath the pectoralis major muscle.
The choice of incision site—whether inframammary (under the breast fold), periareolar (around the nipple), or transaxillary (via the armpit)—is determined by the surgical plan and individual anatomical considerations.
What shape breast implant may be considered?
Breast implants are primarily categorised as round or “tear-drop” shaped (anatomical), with the selection determined by your chest wall anatomy, existing breast tissue distribution, and clinical objectives.
Round implants provide uniform volume and are often utilised to achieve fullness in the upper pole of the breast. In contrast, contoured or “tear-drop” implants are designed with more volume in the lower half to mimic a sloped profile and are frequently used in reconstructive cases or for patients with minimal breast tissue.
During your clinical assessment, Specialist Plastic Surgeon Dr Sophie Ricketts will evaluate these anatomical factors to determine which shape is clinically appropriate for your surgical plan. This discussion includes the specific technical characteristics of each device and their associated risks, such as the potential for implant rotation in contoured models. The goal is to identify the most stable structural approach for your individual anatomy.
What is Breast Implant associated ALCL?
Implant associated ALCL (Anaplastic Large Cell Lymphoma) is a rare form of cancer that develops because of breast implants in the scar capsule around the implant. It is thought to be associated with a very low grade, undetectable infection in this scar tissue. I stick to the 14-point plan to minimise the risk of infection around the implant which includes the used of the Keller Funnel™ allowing a no-touch technique of the implant, antibiotics and nipple shields, to mention a few.
Breast Augmentation: Risks and Complications
Breast augmentation (augmentation mammoplasty) is a significant surgical procedure. While Dr Sophie Ricketts follows rigorous clinical protocols to manage patient risk, all surgery carries inherent complications. It is essential that patients understand these potential risks before deciding to proceed.
General Surgical Risks
-
Anaesthesia Risks: Potential adverse reactions to general anaesthesia, including respiratory or cardiac complications.
-
Infection: Post-operative infection may require antibiotics or, in severe cases, the temporary removal of the implants.
-
Haematoma and Seroma: The accumulation of blood (haematoma) or fluid (seroma) around the implant, which may require surgical drainage.
-
Poor Wound Healing: Risks are higher for smokers or patients with certain pre-existing medical conditions.
-
Deep Vein Thrombosis (DVT): The risk of blood clots forming in the legs, which can be life-threatening if they travel to the lungs.
Implant-Specific Risks
-
Capsular Contracture: The formation of firm scar tissue around the implant, which can cause the breast to feel hard, look distorted, or become painful.
-
Implant Rupture or Leakage: Implants are not lifetime devices. The shell may tear or leak over time, requiring replacement or removal.
-
BIA-ALCL: Breast Implant-Associated Anaplastic Large Cell Lymphoma is a rare but serious immune system cancer that can develop in the scar capsule around textured implants.
-
Breast Implant Illness (BII): Some patients report systemic symptoms (such as fatigue, joint pain, or “brain fog”) which they attribute to their implants.
-
Malposition or Displacement: The implant may shift from its original position, leading to asymmetry or an unnatural appearance.
-
Rippling and Visibility: In patients with thin breast tissue, the edges or folds of the implant may be visible or palpable under the skin.
Sensory and Functional Risks
-
Changes in Sensation: Temporary or permanent numbness or increased sensitivity in the nipples or breast skin.
-
Interference with Mammography: Implants can make it more difficult to see breast tissue during routine cancer screenings; specialised “displacement views” are required.
-
Breastfeeding Issues: Some patients may experience a reduced milk supply or difficulty breastfeeding following surgery.
Mandatory Compliance Information
Important Notice for Patients
Under the Medical Board of Australia’s guidelines for cosmetic surgery:
- GP Referral: You must obtain a referral from your GP before your first consultation.
- Psychological Screening: You will be screened for Body Dysmorphic Disorder (BDD) to ensure surgery is appropriate for you.
- Two Consultations: A minimum of two pre-operative consultations is mandatory.
- 7-Day Cooling-Off Period: After your second consultation, you must wait at least seven days before booking surgery or paying a deposit.
- Second Opinion: Any surgical or invasive procedure carries risks. Before proceeding, you should seek a second opinion from an appropriately qualified Specialist Plastic Surgeon.
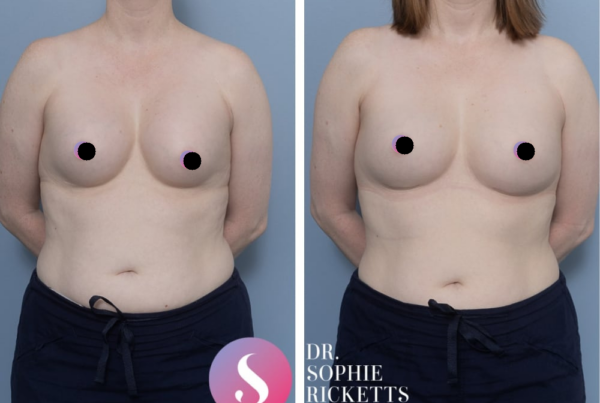
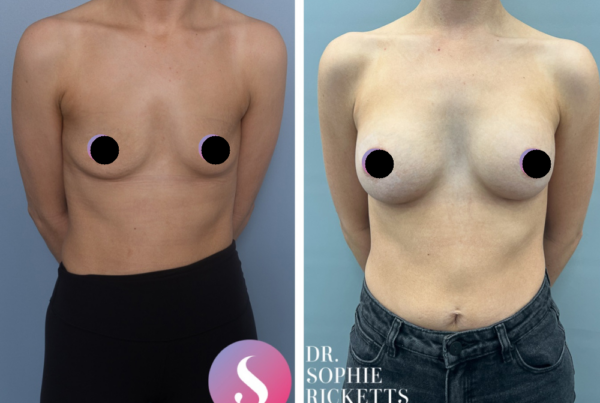
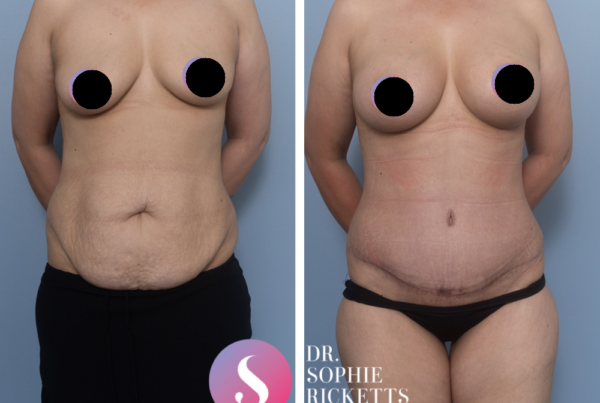
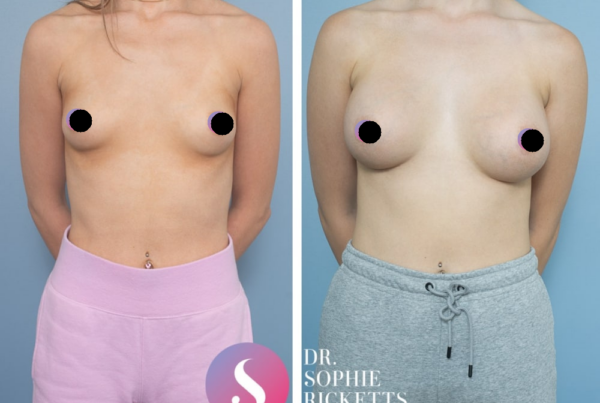
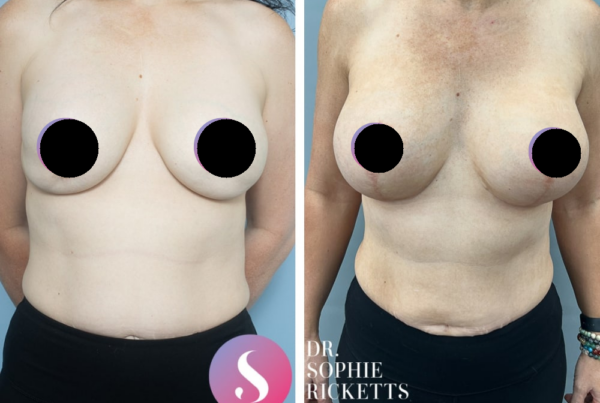
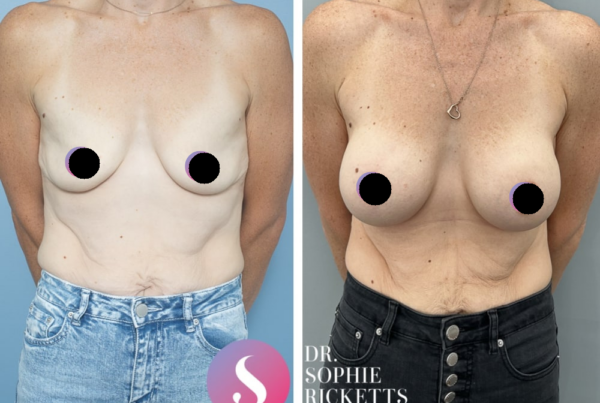
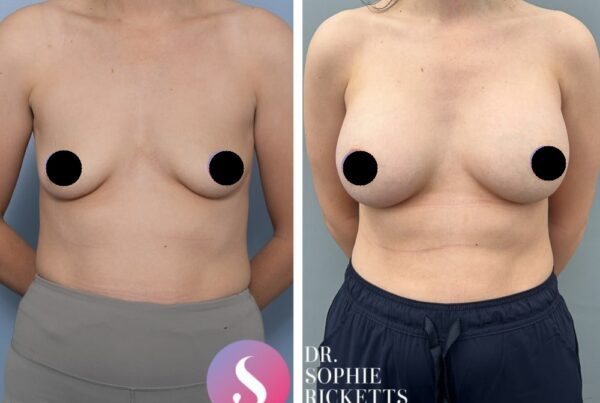
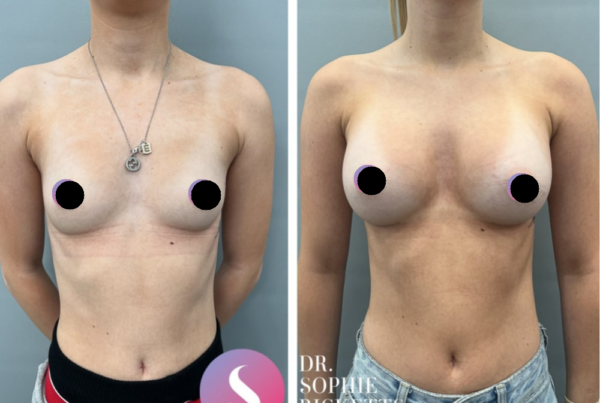
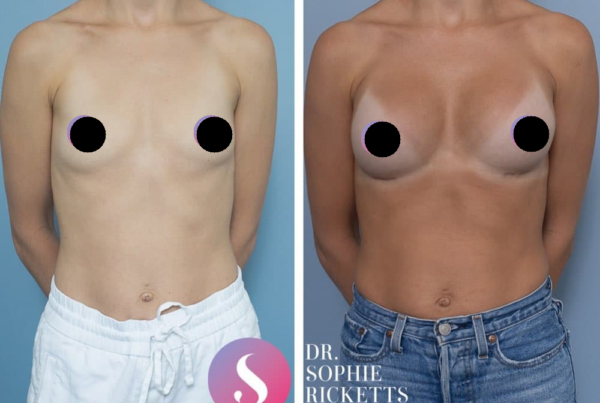
Gallery
Individual results vary. All surgical procedures carry risks and require a consultation to determine suitability.
These images are for illustrative purposes only and do not guarantee a specific outcome. Before proceeding, you should seek a second opinion from an appropriately qualified health practitioner.
FAQ
What is breast augmentation surgery?
Breast augmentation (augmentation mammoplasty) is a surgical procedure intended to address the volume, shape, or symmetry of the breasts using prosthetic implants or autologous fat transfer. Clinical indications for this procedure may include addressing developmental asymmetry, or adding volume lost due to pregnancy or weight changes
How is the procedure performed?
The surgery is performed under general anaesthesia. It involves surgical incisions to create a pocket for the placement of an implant or the injection of processed fat. As with all invasive surgery, there are inherent risks, a required recovery period, and results will vary significantly between individuals.
What happens during the consultation?
In accordance with Australian regulatory standards, the consultation process is a comprehensive clinical assessment. Dr Sophie Ricketts will review your medical history, discuss your motivations, and perform a mandatory screening for Body Dysmorphic Disorder (BDD).
The consultation also covers:
- A detailed explanation of the surgical risks and potential complications.
- Discussion of non-surgical alternatives.
- An overview of the expected post-operative recovery timeline.
A valid GP referral is required before your first appointment, and a 7-day cooling-off period must pass after your second consultation before any surgery can be booked.
Who is a candidate for breast augmentation?
candidates for breast augmentation are individuals who:
- Desire a change in breast size: Candidates should have a clear and realistic expectation of the desired increase in breast size.
- Have fully developed breasts: Breast augmentation is typically recommended for individuals whose breasts have fully developed, which usually occurs in the late teens or early twenties.
- Have good overall health: Candidates should be in good physical health and free from any underlying medical conditions that could pose risks during surgery or impede the healing process.
- Have realistic expectations: It’s important to have realistic expectations about the outcomes of breast augmentation and understand the limitations and potential risks involved.
- Are emotionally prepared: Breast augmentation is a significant decision, so candidates should be emotionally prepared for the procedure, including understanding the potential impact on body image.
During a consultation with a plastic surgeon, they will evaluate a candidate’s physical health, examine the breast anatomy, discuss desired outcomes, and address any concerns. They will also consider factors such as the individual’s breast size, shape, and skin quality to determine the most appropriate surgical approach and implant options.
It’s crucial to have a thorough discussion with a qualified plastic surgeon to assess candidacy, understand the procedure, discuss potential risks, and ensure that breast augmentation is the right choice for the individual’s goals and expectations. See above “Implant specific Risks”.
Can I breastfeed with breast implants?
Breastfeeding after breast augmentation is generally possible, but it can depend on factors such as implant placement and incision location. While many women with implants can breastfeed successfully, it’s important to discuss your desire to breastfeed with your plastic surgeon and consider individual factors that may affect breastfeeding.